We are almost halfway through the year 2020 and the Covid-19 pandemic still continues to wreak havoc in many countries. As of now, about 7.2 million people have been infected including 3.5 million recoveries and 408,000 deaths.
Individuals who contract the virus often don’t show any symptoms, while some experience mild symptoms that are similar to that of the flu like fever, cough and loss of taste. However, the worst-hit patients are often the ones who have difficulty breathing as Covid-19 is a type of coronavirus similar to SARS that causes pneumonia-like symptoms.
These ones have to be isolated in the intensive care unit and put on ventilators to help them breathe. While this machine helps keep them alive, the suffering they have to go through is what most don’t talk about.
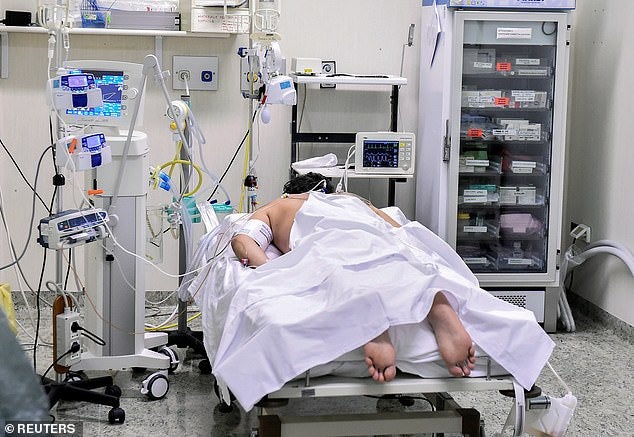
When are ventilators needed
A ventilator basically takes over the body’s breathing process when disease causes the lungs to fail. This gives the patient time to fight off the infection and recover.
A doctor decides to put a patient on a ventilator when they show signs of respiratory failure. The patient’s breathing rate will increase, they will look distressed and the CO2 in the blood goes up and they can become sedated, says Prof David Story, deputy director of the University of Melbourne’s Centre for Integrated Critical Care.
He says that a normal breathing rate is about 15 breaths a minute and if the rate goes up to about 28 times a minute, this is a signal that ventilation may be needed.
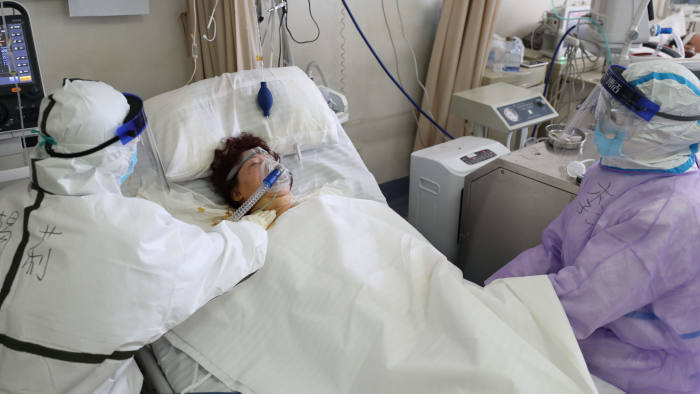
How ventilators work
In order to put a patient under ventilation, doctors will perform a procedure called “intubation”, where the patient is sedated and given a muscle relaxant. An endotracheal tube is then placed through the mouth and into the windpipe and is attached to a ventilator that monitors how much oxygen is pushed into the lungs.
The ventilator also has a humidifier, which adds heat and moisture to the air supply so it matches the patient’s body temperature, reported BBC citing the World Health Organisation.
If placing the tube through the nose or mouth proves to be difficult or is not helping the patient, an opening is made in the patient’s neck and a tracheostomy tube is placed through that hole, according to the National Heart, Lung and Blood Association (NHLBA).
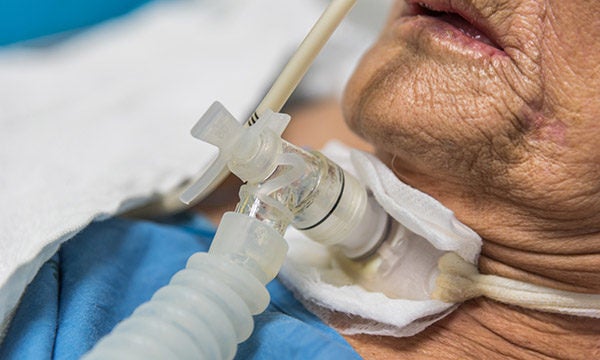
The painful truth about ventilators
However, prolonged use of ventilators poses other health risks for the patient. First off, the breathing tube makes it hard for patients to cough, allowing bacteria to enter their lungs which could lead to pneumonia. As if Covid-19 patients don’t already have problems with their lungs, ventilators may cause additional problems.
According to NHLBA, these are some of the additional problems that patients on ventilators could face:
- Atelectasis – a condition in which the lung does not expand fully. This causes the air sacs to collapse.
- Blood clots – staying in one position for long periods of time can cause blood clots and serious skin infections.
- Lung damage – pushing too much air into the lungs or with too much pressure can harm your lungs. Too much oxygen can also damage your lungs.
- Muscle weakness – ventilators take off the load from your diaphragm and other breathing muscles, causing them to become weak.
- Vocal cord damage – since the breathing tube is placed through your nose or mouth into the windpipe, the tube can damage your vocal cords.
- Fluid buildup – the air sacs inside your lungs, which are usually filled with air may fill up with fluid. This is called pulmonary edema.
- Pneumothorax – a condition in which air leaks out of the lungs and into the space between the lungs and the chest wall. This can cause pain and shortness of breath. It may cause one or both lungs to collapse.
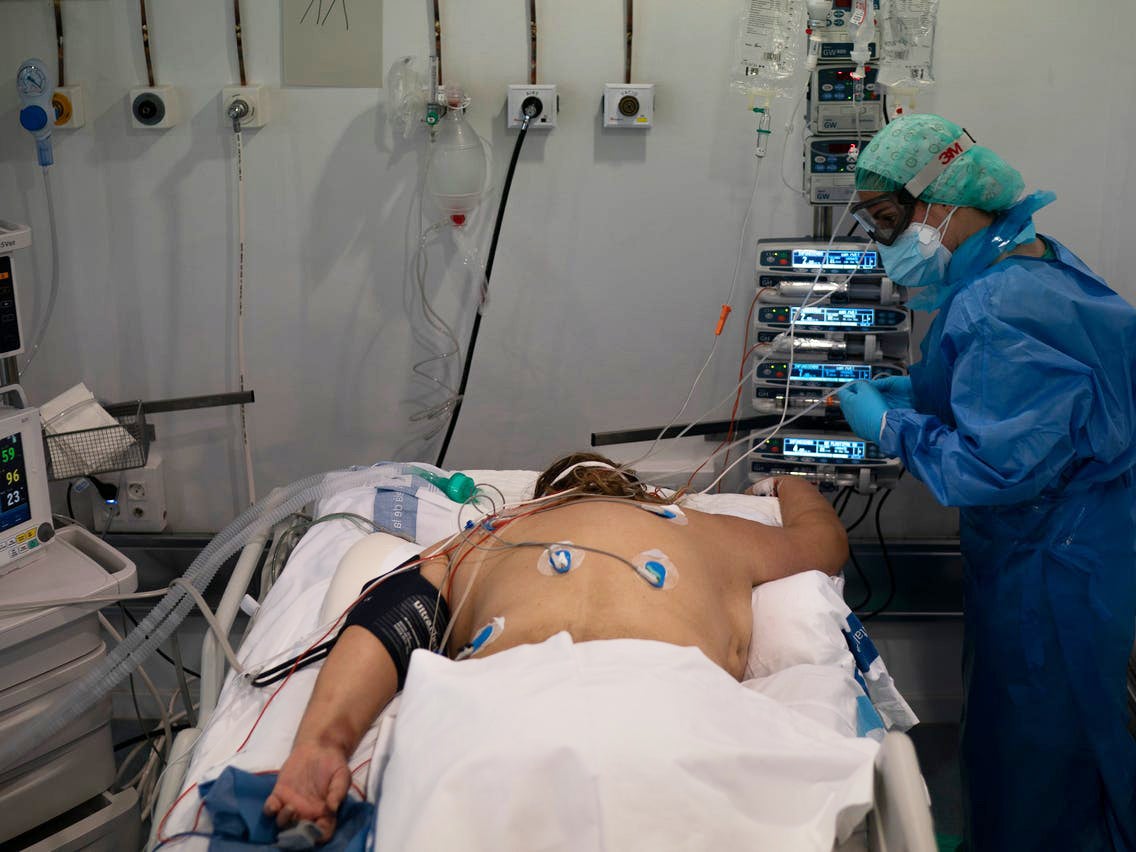
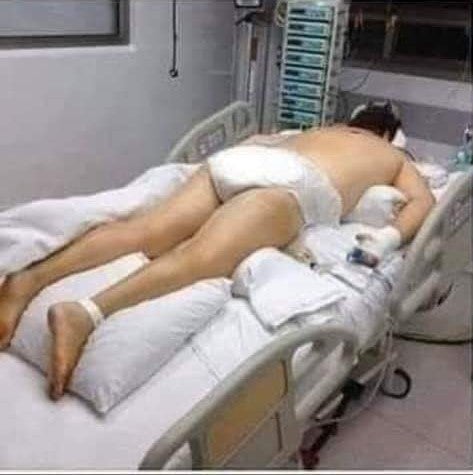
Furthermore, Covid-19 patients on ventilators are often placed on their stomachs to aid blood flow through the lungs, helping better match the airflow to the blood supply, says Dr. Greg Martin, a professor of pulmonary critical care at Emory University and president-elect of the Society of Critical Care Medicine.
Not forgetting that patients can no longer perform basic daily functions like eating and going to the bathroom on their own, this means that they have to wear diapers or be connected to a catheter.
Dr. Burton Bentley II, CEO of Elite Medical Experts told Business Insider that sometimes, patients’ lungs resist the machine, and they have to be put in a medically induced coma.
This probably does not even come close to what critical Covid-19 patients on ventilation actually experience, but we must never forget that this is what thousands of people all around the world have to go through.
As Malaysia slowly reopens its economy and restrictions are lifted one by one, let us remember that we are not safe from Covid-19. Therefore, we need to take care of ourselves and our loved ones and follow standard operation procedures set by the government.
The future of Malaysia depends on you!
Also read: Viral Video: Malaysian Frontliners Cheer & Clap As We Move Into RMCO